Safety is the number-one concern for behavioral health staff and leadership at ERs and hospitals. But traditional systems, like paper clipboard rounding and electronic clipboards, still put staff and patients at risk. ObservSmart digital solution can ensure validated compliance with patient safety checks, and behavioral health facilities should invest in a tech-enabled system that was made specifically for mental health settings — and designed by behavioral health professionals.
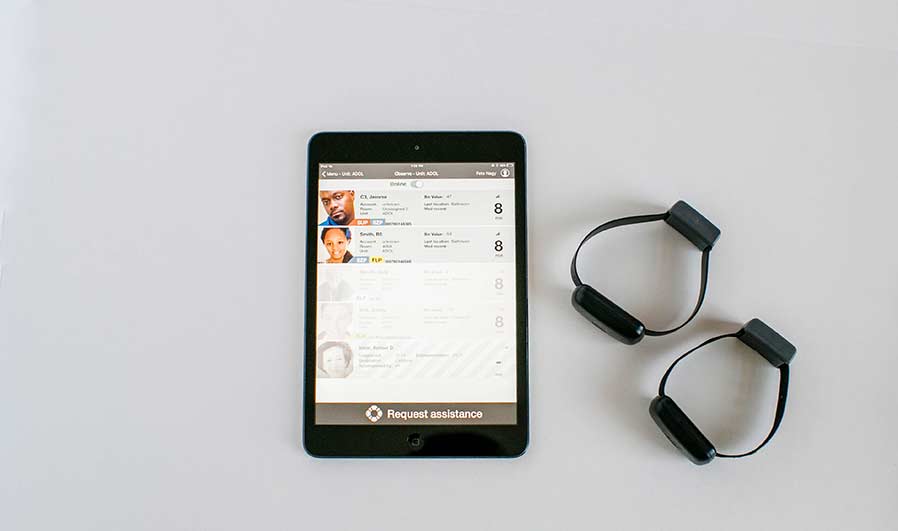
InvisALERT’s ObservSMART system helps staff maintain observation compliance in residential, substance abuse, ERs, and behavioral health units. This innovative proprietary software works with patented, highly tamper-resistant wristbands to improve compliance, increase the quality of care, and ensure the safety of both staff and patients.
Curtis Cornish, Director of Clinical Operations and Implementation, shares why InvisALERT’s innovative technology and a passion for improving lives brought him out of retirement, and how the system is revolutionizing mental health treatment.
Q: What is the history of InvisALERT?
A: I have been with the company for about five and a half of the six years that the company has been around. I was the first employee hired, so I’ve been able to watch it grow to over 25 employees.
Q : What is your background? Do you have experience in healthcare?
A : I have worked in mental health for over thirty years. I joined the Army out of high school as a Military Intelligence Analyst. After the military, I attended college while working at the Post Office and as a mental health tech. From there, I graduated with a dual degree in Electronics and Robotic Engineering.
I went back to school to become an LPN and later for my RN. I was Director for Nursing Services at the Jane E. Mitchell Forensic Unit for the State of Delaware, where I retired in 2010.
Q : What is your current role with InvisALERT?
A : I am the Director of Operations and Implementation and I’m in charge of the training and implementation team. We lead onsite training and implementation of the ObservSMART system.
This includes training site staff, helping leadership develop policies, reviewing best practices, and implementing management processes to support the system and achieve the best outcomes.
I have a clinical background, so I give input with all new product developments and reviews, too.
Q : How did you first learn about ObservSMART?
A : Although I retired from nursing, I must work several hours a year to remain a licensed nurse. I met the CEO of InvisALERT during his first ObservSMART pilot at a local behavioral health hospital. He was impressed with my leadership skills and experience, so he offered me the position I’m in currently.
Q : After being retired for so long, why did you think this was a good move at the time?
A : I had been retired for five years before I learned about InvisALERT. I retired so young but never planned on staying retired. Even then, it was an adjustment.
I had supervised staff in the past as a director and a charge nurse, so I was very familiar with how critical the paper clipboard system is for people in mental health. Rounding and doing observation is — hands down — the most crucial leadership responsibility in the hospital.
However, we often give that responsibility to the least qualified and least paid individuals in the hospital and do not give them the tools they need to be successful. So it’s a big deal. Having one-on-one face-to-face interaction every 15 minutes is the most important responsibility in the hospital. I wanted to be part of the solution.
Q : What does customer success look like to you?
A : The ObservSMART system is very intuitive. It’s easy to learn, and once we implement it, it’s clear from the beginning that our software and hardware ensure patient safety.
But that’s 50% of our approach to customer success. The other half of the puzzle is helping clients use this new safety initiative successfully.
What do their policies and practices look like? Are they realistic?
Hospitals want every box checked. They want all of the rounds checked every 15 minutes, and in my experience, there’s no way to check every box with those parameters with what they are using now. So many things are out of our control. We can’t control when a patient hides under their bed, for example.
Customer success means making hospital leadership realistic. Their goals and compliance standards need monitoring for success, but those goals have to be realistic and they need to give the staff the tools they need.
Part of my role is implementing the system, but more importantly, helping the department with post-implementation. We look at their progress and leadership, so they stay successful. What events have happened in the hospital? The system holds everyone accountable and makes you improve on those things. This system gives the client the tools they need to succeed.

Q : What are some challenges you come across when it comes to implementation (i.e. technology, resistance, etc.)?
A : We work with the existing IT department and clinical leadership to implement the system.
The hospital can use our system as a standalone solution because it can discharge, admit, and observe patients on its own. We can also build an interface where, once you admit it in the EHR system, everything pops up automatically, so you don’t have to admit directly on a tablet.
We have unique challenges with staff and training. We are capable of training 120 staff members in a day and a half, which is pretty intense. It’s a challenge for our clients to train those 120 people in a short period of time. But we set them up with a complete training platform, so they can manage new hire training or people with struggling performance after implementation.
We assist clients to learn proper banding of patients. In our system, when the patient wears the band, it’s part of a compliance system. That means you cannot make an observation until you’re in proximity of the patient that the hospital determines. This ensures that the tech actually saw the patient.
Hospitals want staff to step into a patient’s room to check on their well-being. Our system’s proximities push the staff to enter that room. Sometimes they’re uncomfortable visiting patient rooms while they’re sleeping, so we have to work with staff to help them understand that checking on patients every 15 minutes is an essential safety concern.
The biggest challenge is changing the culture behind ingrained negative behaviors. The system will point out any workflow, performance, or teamwork issues during implementation.
Q : How do you improve patient safety?
A : Patient safety has always been a major concern for me as a staff nurse, supervisor, and director. My greatest fear is any harm coming to the patients. This conditioned me to ensure that my staff has the right training.
I have also put systems in place to ensure consistency. An assignment sheet is a simple way to designate roles and responsibilities. These processes must be in place to keep staff focused, responsible, and accountable. With every install I do of the ObservSMART system, I leave the facility knowing their patients are safe.
Q: What would you consider to be proper bedside manner/professionalism?
A : The behavioral health industry requires that staff maintain a high degree of professionalism. If a staff member is unprofessional, patient populations will often lash out and create conflict.
If patients have depression or struggle with suicidal thoughts, unprofessional interaction can be a trigger for the patient to harm themselves. The staff needs to be aware of patient stressors. If not, it can cause a lot of conflict in a psychiatric unit.
Q : What is the best way to be an advocate for loved ones?
A : A family member can be an advocate by understanding admission and discharge criteria if your loved one struggles with mental health issues or substance abuse.
Families should support the hospital team when it comes to any measure that focuses on patient safety. Ask the facility if they use ObservSMART. Ask what their protocols are for making sure their loved one is safe. Discharge criteria include:
- The patient can care for themselves.
- The patient makes safe choices.
- The patient copes with frustration positively.
Q : How does the use of the ObservSMART system change things for the staff?
A : ObservSMART is a compliance system, which means that it validates whether you completed the observation.
You can’t complete the observation unless you’re within the proximity set by the system and by hospital leadership. It’s an accountability system. The supervisor can monitor on or off-site as to whether you are on time with your rounding. There are alarms for missed checks so that supervisors can react right away.
When implemented, we see a reduction in sentinel events, falls, and victimization in mental health, residential, or nursing home settings.
Q : How is ObservSMART different from other healthcare technology?
A : ObservSMART is different because other health care technology plays more of a supportive logistical role in healthcare. The ObservSMART System is a critical system used by the clinical staff to keep patients safe.

Q : What problems does ObservSMART solve?
A : Once the system is implemented, it immediately helps hospital staff identify teamwork problems, workflow issues, staffing needs, policy deficiencies, and poor management processes.
Unlike clipboard and paper rounding, ObservSMART keeps staff attentive. It prompts them to reach out to their peers and nurses when they are overwhelmed with patient care. It also gives leadership objective data to review compliance standards.
Q : What is the feedback from customers and the biggest selling points?
A : Our clients adore the system. They often say, “We thought a bunch of tech guys would be training us and telling us how to do our jobs, but you guys know what we deal with every day.”
The ObservSMART system was designed by mental health providers, for mental health providers. It’s intuitive and easy to learn, the data is objective and holds people responsible, and the patients are safer. The system is adaptable, too. It can operate as a standalone system, or we can interface with any hospital’s EHR system.
Q : What should decision makers in hospitals and ER departments know about the ObservSMART system?
A : People go to behavioral health hospitals and ERs for medical and psychiatric distress. Because of that, it is easy for staff to become overwhelmed and distracted.
Patients in a behavioral health hospital are required to interact and go to groups. It’s often hard to keep track of all of these moving pieces and manage high acuity from a crisis. These healthcare workers need reliable compliance tools driven by technology to help them do their job.
The 1:1 ObservSMART system has three mechanisms to ensure that staff is attentive to the most critical patients on the unit or ER. Staff wear an armband and must complete an observation, they must frequently move as not to fall asleep, and lastly, they must be near the patient at all times.
Any one of these infractions will notify the staff first, and if they do not correct the violation, the system notifies hospital leadership. It’s simple but sophisticated and effective.
Q : What is the post-implementation process and time frame? What are you hearing from staff?
A : We typically go in on a Monday and see all of the patients by Tuesday evening.
On Wednesday and Thursday, we do implementation rounding with our system. By Thursday afternoon, we can give the client feedback on their compliance numbers. We want to see compliance roundings and face-to-face interactions at 98% that day.
We measure other indicators, too. The system looks at forced observations, how the team is using the system, and the maximum amount of time it takes to go around the unit.
We typically have anywhere between 98-100% banding of patients before we leave the hospital on Friday. We are very successful at achieving compliance levels within the first week of implementation.
Q : What are some challenges faced in banding the patients? What is some advice or training you would give the staff to best handle possible challenges?
A : Once we train staff on banding techniques, they must continue training. Patients continue to come in and receive their bands for allergies or medication.
What’s challenging is the concept of treatment compliance. We’ve noticed that hospitals with centralized intake and admissions do better at banding than hospitals that admit directly to a unit, so the success rate is much higher in a hospital with an admissions unit.
They have a dedicated core group of folks that understand banding and do it often. Today, all hospital staff have to work at banding across different units. When banding doesn’t happen in a centralized area, the training can be watered down.
I think of this as compliance with treatment. Some patients come in and aren’t compliant with all aspects of their treatment. Non-compliant patients are the ones that are not happy with their treatment and acting out. These violent folks are causing violent codes because they push back against treatment.
You need their buy-in for everyone’s safety, which means wearing a band. Our system includes banding because we want hospitals to have a plan to get patients banded. But they need to have a plan with non-compliant patients. That starts with staff members connecting and building rapport with patients. If you develop a relationship with a patient and they believe you are invested in their well-being, they are more likely to buy into treatment and less likely to cause conflict.
Q : Are there mental health resources for staff?
A : Staff have a benefits package that includes mental health and substance abuse resources. They simply dial a number to reach out on their own, or they can get a referral from me.
Q : Do you have any final thoughts you want to share?
A : I have seen very few hospitals with systems designed for behavioral health, by behavioral health folks. The ObservSMART system alerts the staff members first and then supervisors, if not corrected. ERs and hospitals must give their staff the best tools to keep themselves and their patients safe.
Patients and staff need a safe environment in which to seek treatment and do their jobs, respectively. ObservSMART revolutionizes patient safety checks by helping hospitals reduce risk, errors, and costs. Contact us to schedule a demo to find out what our innovative compliance technology can do for you.